| Table of Contents |  |
|
Original Article
| ||||||
| The effect of neuromuscular electrical stimulation (Firefly™ device) on blood lactate clearance and anaerobic performance | ||||||
| Darryl J. Cochrane1, Catherine Teo2 | ||||||
|
1Ph.D, Massey University, School of Sport & Exercise, Palmerston North, New Zealand.
2BSc, Massey University, School of Sport and Exercise, Palmerston North, New Zealand. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Cochrane DJ, Teo C. The effect of neuromuscular electrical stimulation (Firefly™ device) on blood lactate clearance and anaerobic performance. Edorium J Sports Med 2015;1:1–6. |
|
Abstract
|
|
Aims:
To examine the effectiveness of the neuromuscular electrical stimulation (NMES) device to determine its ability during acute recovery to hasten blood lactate (BLa) clearance and enhance anaerobic performance.
Methods: In a randomized, crossover design, nine healthy participants (6 males and 3 females) performed a Wingate cycle test followed by 30 min recovery of either neuromuscular electrical stimulation (NMES) or passive resting (PAS) proceed by another Wingate test. Blood lactate concentration was measured during the 30 min recovery phase. Results: Both PAS and NMES showed a significant decline (p<0.01) in BLa but NMES did not hasten BLa removal any faster compared to PAS. Likewise, there was no significant difference (p>0.05) in Wingate performance with the exception that mean power was significantly reduced (p>0.05) following NMES. Conclusion: Using the NMES device as an acute recovery strategy (30 min) did not accelerate BLa removal and showed no performance enhancement compared to PAS. | |
|
Keywords:
Acute recovery, Blood lactate, Peroneal nerve, Wingate cycle test
| |
|
Introduction
| ||||||
|
Neuromuscular electrical stimulation (NMES) is a technique that delivers electrical impulses through an external device that is connected to surface electrodes, which are placed on the skin in proximity of the skeletal muscle motor point to elicit visible muscle contractions [1]. The application of NMES has been prominent in sporting and medical disciplines for physical training and rehabilitation to improve and/or preserve muscle function for athletes, healthy and compromised populations [2]. Recently, NMES has gained further acclaim by athletes and trainers as a potential modality to accelerate the recovery process from short and long-term bouts of exercise. The ability to recover from exercise bouts and training sessions without the residual fatigue is of great interest to athletes and coaches for maintaining high levels of performance. As a consequence of high intensity exercise bout(s), peripheral fatigue develops resulting in considerable metabolite accumulation (Glaister, 2005) that may disturb the contractile process [3] [4] and affects subsequent performance [3]. It has been documented that active recovery through its increase in blood flow can expedite blood lactate concentration (BLa) removal and return the body to basal levels faster than passive recovery [5] [6]. Therefore, NMES provides a sound basis as a recovery strategy through its ability to induce muscle contractions with minimal metabolic (energy) cost to promote blood flow, which has the potential to accelerate metabolite removal and facilitate the recovery process. Previous research has observed that NMES can hasten BLa clearance faster than passive rest during an acute recovery phase (20–30 min) in various athletic populations [7] [8] [9] and enhances anaerobic rowing performance [10]. In contrast, using NMES during 30 min recovery from supramaximal exercise did not accelerate BLa [11] and no improvements have been reported in isometric force, lower limb power [10] and anaerobic cycling performance [11] in comparison to passive resting. The discrepancy in findings may be explained by the protocols, equipment and location of the stimulation to maximize its effectiveness. Recently, a new technique of electrically stimulating the peroneal nerve with mild activation was observed to significantly increase femoral vein blood flow [12]. This ability to increase limb blood flow has implications for accelerating the recovery process following high intensity exercise by removing accumulated metabolites and decreasing intracellular fluid volume [13]. As a result of these findings, a new device has been commercially developed, known as Firefly™, it has been purported to elicit the aforementioned responses to enhance recovery and improve performance. Unlike its predecessors, it is portable, wireless and easy to administer. This should appeal to athletes that require convenience to apply a recovery modality that is not restricted by time, space and specialized equipment. To date, the use of NMES Firefly™ device has only focused on recovery periods of 24 hours post-exercise [14] or longer [15]. Nonetheless, a recovery time of less than one hour has importance for athletes who have multiple event heats that are performed on the same day [11] and for sportspeople that want to expedite the recovery process when undertaking repeated bouts of high-intensity, short-duration exercise. To our knowledge there has been no study that has investigated the use of this novel NMES device during acute recovery (< 1 hr) following a high-intensity, short-duration exercise bout. Therefore, the aim of this study was to examine the effectiveness of the NMES Firefly™ device (OnPulseTM Technology, Firstkind Ltd, Cheshire, UK) to determine its ability during acute recovery to hasten BLa clearance and enhance anaerobic performance. Given the intention that this NMES device can activate the peroneal nerve by influencing local blood flow to increase the removal of accumulated metabolites from the stimulated ankle and foot muscles, it was hypothesized that NMES would be more effective than passive resting to hasten BLa clearance during recovery and enhance anaerobic performance following a high-intensity, short-duration bout of stationary cycling. | ||||||
|
Materials and Methods
| ||||||
|
Participants Study Design Participants attended the university's exercise laboratory on three separate occasions. On the first visit, participants were familiarized with the Wingate cycle test and the NMES device (Firefly™, FirstKind Ltd, UK), where participants' self-selected a level of stimulation intensity to elicit a tolerable and comfortable muscle contraction [10], which was noted for the NMES treatment. For the following two visits, participants performed a warm-up (100 W) on an electronically braked cycle ergometer (Lode Excalibur Sport, Groningen, The Netherlands) for 3 min with 1 min of rest before undertaking a 30 s Wingate test (Pre-recovery). This was immediately followed by a 30 min recovery intervention consisting of either passive resting (PAS) or NMES, the order of which was randomly assigned, prior to a repeat of the Wingate test (Post-recovery). The 30 min recovery was selected because it is relevant to many sporting scenarios that consist of events or heats and/or repechages that are less than one hour apart [11]. Participants were informed to maintain their normal nutritional intake and refrain from physical activity and ingesting caffeine 24 hr prior to visit 2 so it could be replicated for visit 3. Seven days separated each testing session and to account for daily biorhythms testing was conducted at the same time of day. A 3% change in anaerobic performance would be considered small but a worthwhile difference, with a power of 0.75 and a = 0.05, a power analysis revealed that nine participants would be sufficient to detect such changes. Recovery Treatments Wingate Testing Statistical Analyzes | ||||||
|
Results | ||||||
|
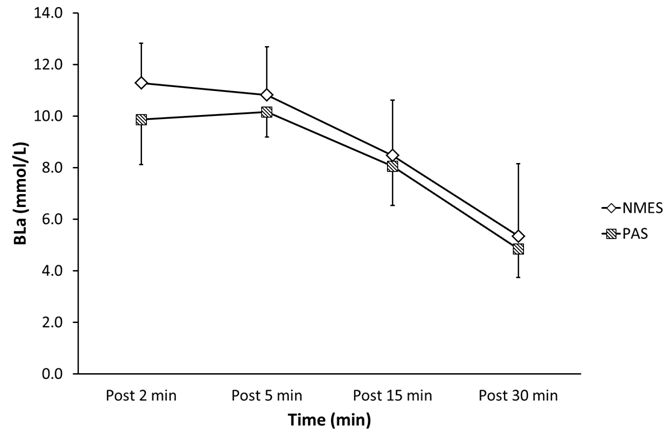
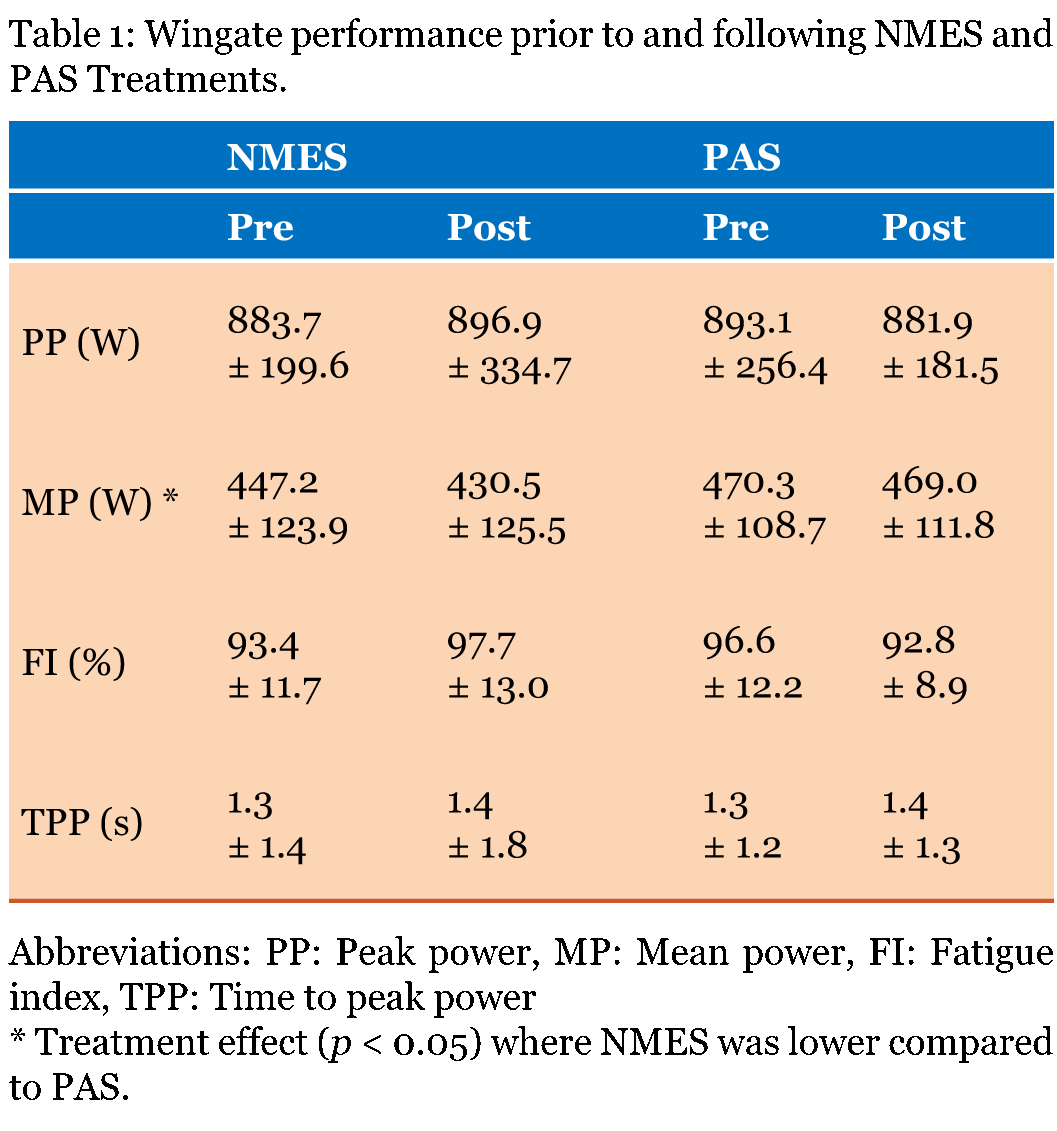
For BLa there was a main effect, such that during the 30 min of recovery there was a significant decline (p<0.01) but NMES did not hasten BLa clearance any faster compared to PAS (Figure 1). Additionally, there was no significant difference (p>0.05) of BLa between treatments at the start of the recovery phase (post 2 min) and there was no participant effect (p>0.05) on BLa clearance. For the performance parameters of PP, FI and TPP there was no main or interaction effects (p>0.05). However, there was a treatment effect where the MP was significantly lower following NMES (p=0.042) compared to PAS (Table 1). | ||||||
| ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
The main findings of this study were the NMES Firefly™ device did not hasten BLa clearance and MP declined significantly compared to PAS but no other performance changes were evident following a high-intensity, short-duration bout of exercise. The manufacturer of the NMES device claim that it increases blood circulation to accelerate the removal of metabolites, enhance leg muscle recovery and reduce delayed onset of muscle soreness. Due to its ability to activate the peroneal nerve and stimulate the lower leg muscles to promote local blood flow, the expectation was that the Firefly™ device would accelerate BLa during the 30 min recovery compared to PAS. However, despite BLa being significantly reduced, there was no difference in its removal between NMES and PAS. Previous NMES Firefly™ studies have also reported little effect in accelerating BLa following intense intermittent exercise [14] [16]. Other short-term recovery (= 30 min) studies that have used NMES devices of a hand-held unit connected surface electrodes have reported enhanced [7] [8] [9] or no change [11] in BLa clearance compared to PAS. It has been reported that directly stimulating the triceps surae provides an additional muscle pump to increase lower-limb blood flow to facilitate venous return [17]. However, in the present study the NMES device was positioned according to the manufacturer's instruction above the popliteal fossa of the knee joint to stimulate the common peroneal nerve to activate the muscles of the ankle dorsiflexors and foot evertors. It is possible that the Firefly™ device may not have had the desired effect because the triceps surae were not directly stimulated to elicit the required muscular contractions to promote blood flow and venous return; therefore, stimulating larger muscle mass, such as the quadricep and hamstring groups may be of more benefit. The initial high level of post-exercise BLa exhibited in the current study is in agreement with other studies that have investigated the efficacy of various recovery strategies following strenuous exercise bout(s) [7] [9][11]. High-intensity, exercise is often associated with peripheral fatigue where additional metabolite accumulation [18] [19] may change various cellular mechanisms that has a direct effect on the contractile process to influencing subsequent performance [3]. It has been well documented that active recovery can accelerate BLa clearance compared to passive recovery [6] [20] [21] [22]. Low intensity recovery exercise is able to elicit muscle contraction, which promotes a pumping action that may influence hemodynamics to facilitate the shuttling and removal of metabolites and reduce localized edema [23]. However, it is equivocal whether there is a relationship between BLa clearance and subsequent performance. In previous passive and active recovery studies BLa levels have been accelerated with a concomitant performance improvement. [5] [24]. But other research has shown that despite lowering BLa levels during active recovery performance has not been enhanced [6] [25]. Similarly, it has been observed that 30 min of active recovery between supramaximal bouts of cycling significantly expedited BLa clearance following NMES compared to PAS but it did not improve performance [11]. Therefore, increasing BLa removal may not be an appropriate indicator in determining the quality of recovery and accelerating lactate clearance because it does not necessarily translate to a superior performance [26]. One of the most important NMES parameters is the intensity of the electrical stimulus [27], where a greater stimulus should elicit a larger muscle contraction to increase local blood flow and remove metabolites at a faster rate. In the present study, the current pulse of 27 mA with a pulse width between 100–140 µs may have been an inappropriate level to increase localized blood flow and accelerate BLa, which may explain the non-significance findings between NMES and PAS. Likewise, NMES had no effect on PP, TPP, FI cycling performance compared to PAS, which is supported by Malone et al. [11], although the muscle site (quadriceps and hamstrings) and type of NMES (Firefly hand-held NMES unit) were different between the studies. Similarly, in comparison to passive recovery, another type of NMES device had no effect on vertical countermovement jumping and knee extensor strength but improved 30 s rowing performance [10]. In a follow-up study, the same NMES device was administered during a 15-min recovery where shuttle run distance was enhanced compared to active and passive modalities [7]. Nonetheless, in the current study it is difficult to elucidate why MP was the only performance factor to be significantly lowered following NMES compared to PAS. It is possible that NMES placement may had little effect to promoting a muscle pump action to accelerate BLa. However, for this particular cohort, who were recreationally trained the intensity of stimulus may have elicited a small degree of muscle fatigue, which could have resulted in a reduced ability to maintaining a high level of power output during the Wingate. Currently, there is no agreement for prescribing the optimal stimulation, although it has been reported that the optimal pulse duration should be between 100–500 µs [28]. The apparent discrepancy between current and previous findings may be explained by the variances in research methodology including; stimulation intensity and duration, electrode placement, muscle site, recovery time, type of activity to induce fatigue and/or muscle soreness and participant characteristics. A recent systemic review [28] reported a considerable variation in NMES parameters, where stimulation frequency ranged from 1–8 Hz; pulse duration 125–500 µs and pulse intensity of 17.5–92 mA. Additionally, various muscle stimulation sites have been used (quadricep, forearm, and calf) and the duration of the recovery intervention has varied from 6–60 min. According to Malone et al. [28], the use of different NMES equipment is a major contributor for the reported disparity in pulse frequency, pulse intensity, electrode size and positioning. This may account for the lack of consensus in determining the optimal NMES parameters during exercise recovery. | ||||||
|
Conclusion
| ||||||
|
The results of the current study indicate that using the neuromuscular electrical stimulation (NMES) Firefly™ device as an acute recovery strategy (30 min) was unable to hasten blood lactate clearance with no changes occurring from anaerobic cycling performance. However, mean power was reduced following NMES compared to passive resting. There were no adverse effects from using this device and future research should investigate its acute, short-term efficacy to enhance blood flow to promote muscle recovery. | ||||||
|
Acknowledgements
| ||||||
|
We wish to thank the participants in giving their time to volunteer for this study. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Darryl J. Cochrane – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Catherine Teo – Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2015 Darryl J. Cochrane et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|